اقدامات قبل از جراحی بینی + راهنمای کامل
جراحی بینی، به عنوان یکی از متداولترین عملهای زیبایی، در میان افراد با انگیزههای مختلف رواج دارد. فارغ از هدف

جراحی بینی، به عنوان یکی از متداولترین عملهای زیبایی، در میان افراد با انگیزههای مختلف رواج دارد. فارغ از هدف

تا به حال فکر کرده اید که انتخاب یک جراح بینی خوب می تواند چه تاثیر در نتیجه رینوپلاستی داشته

جراحی بینی، یکی از محبوبترین عملهای زیبایی در دنیاست که بسیاری از افراد برای تغییر فرم بینی خود و دستیابی
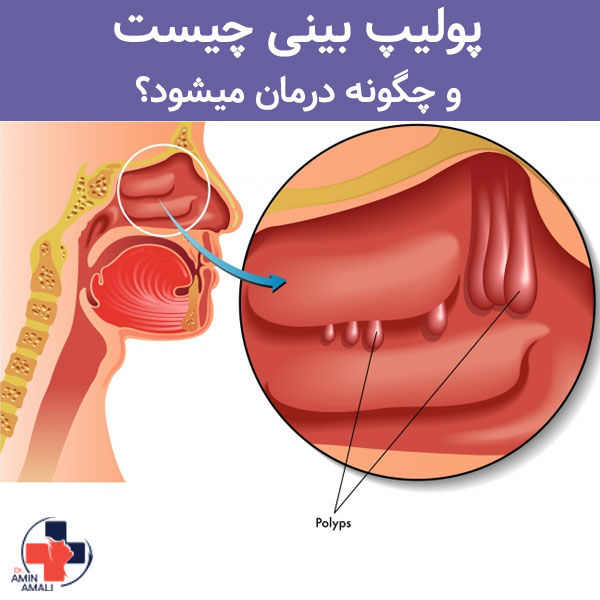
آیا تا به حال حس کردهاید که بینیتان به طور کامل مسدود شده و نفس کشیدن برایتان دشوار شده است؟

یکی از مواردی که برای عمل کردن بینی همیشه در نظر گرفته می شود، هزینه ای است که باید بابت

در دنیایی که تناسب و زیبایی همواره در صدر ارزشها قرار دارند، بینی به عنوان عنصری محوری در چهره، نقشی

بعد از عمل بینی ، وظیفه شماست که از بینی جراحی شده تان مراقبت کنید. البته پس از اتمام

تغذیه بعد از جراحی بینی ، شاه کلید ریکاوری سریع و بیدغدغه است. با انتخابهای غذایی درست، میتوانید تورم و

جراحی بینی نیمه فانتزی، انتخابی ایدهآل برای کسانی است که میخواهند ظاهری متعادل و جذاب داشته باشند. این مدل جراحی،

دکتر امین آمالی، متخصص گوش، حلق و بینی، جراحی زیبایی بینی و صورت، جراحی اندوسکوپی بینی و سینوس، جراحی اختلالات خواب و فارغالتحصیل دانشگاه علوم پزشکی تهران بوده ، دوره تکمیلی در دانشگاه استنفورد آمریکا را گذرانده است.